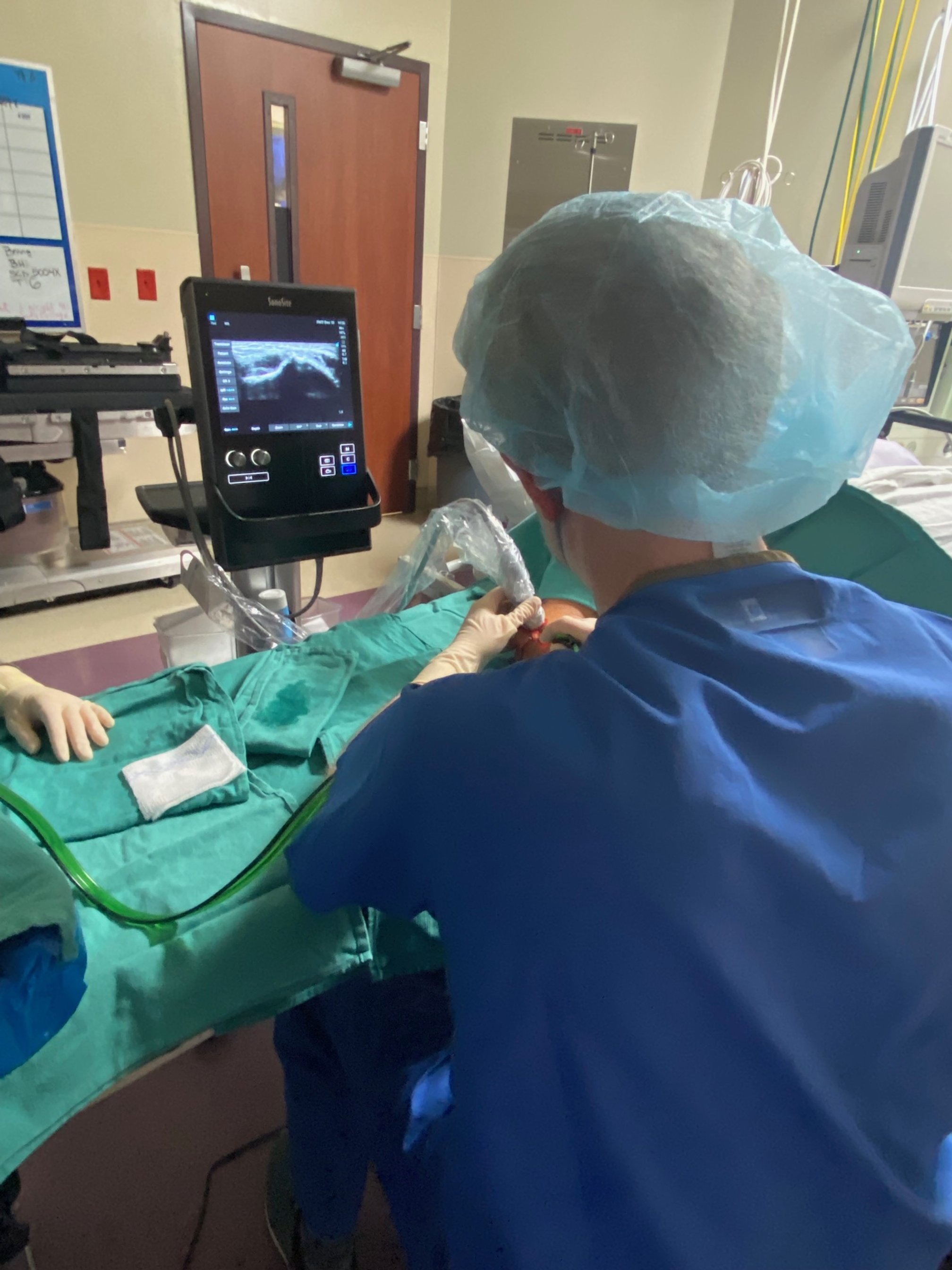
Platelet-rich plasma injections, commonly known as PRP, have been utilized in orthopedics for at least the past 15 years. The first studies in orthopedics looked at PRP being utilized for tennis elbow, and the results were promising.
Fast forward 15 years and now platelet rich plasma has become a mainstay in the treatment of many orthopedic conditions, ranging from osteoarthritis to tendon and ligament problems. An estimated 60% of orthopedic practices now offer PRP to their patients and while some physicians can claim true expertise in this type of treatment, other practices remain novices when it comes to the application of PRP.
Now, to answer the question in the title of this blog, “why do insurance companies not cover PRP….” We will provide an educated opinion with several bullet points.
-Many insurance companies claim that PRP injections are “experimental.” Experimental is a very broad term that can be applied in numerous ways. What classifies something as experimental? In my opinion, this is something that has been utilized for a very short period of time and has very few studies or anecdotal pieces of evidence to demonstrate a sustained rate of efficacy. Meaning, this treatment hasn’t been used for very long, has not been used on very many patients, and we really don’t know what the short-term or long-term results are.
When it comes to PRP, I would say we are light years beyond the experimental stage. For many years, PRP has been used not only in orthopedics, but also in plastic surgery, wound care, dermatology/aesthetics and hair-loss situations, to just name a few. PRP has demonstrated a long track record of safety, and the overwhelming majority of studies demonstrate that patients benefit from these procedures. So, in my mind as a physician of nearly 25 years who has studied medical data for his entire career, I would no longer classify PRP broadly as experimental. Are more studies regarding PRP necessary? Of course. Yet this is true for every treatment in medicine. Trust me when I tell you that there are numerous treatments in all fields of medicine being utilized right now that have been studied far less than PRP.
-Next, the truth is that insurance providers these days are looking to pay for fewer and fewer of your medical expenses. We have to get away from the mentality that “I have health insurance, and it should cover all of my medical needs.” In truth, we are probably getting back to a model where insurance should be used for major health expenses and catastrophic situations, not for most of your routine day-to-day medical care. Almost all of private insurance companies are for-profit organizations. There’s nothing wrong with that. However, you must realize that their first goal is making a profit to sustain their business. Their first priority is not providing the optimal care for the patient, as often is the case, the optimal care is not the least expensive. So, we are constantly preaching to our patients these days that the best treatments in orthopedics are not necessarily the ones you can expect your insurance to cover.
-Finally, to partially take the side of the insurance company, an argument against covering PRP would be that it cannot be “standardized.” We can standardize a medication or certain forms of medical equipment, but we cannot standardize a patient’s blood. Therefore, one person’s PRP may not look like another patient’s PRP, meaning the number of platelets, white cells, etc. may be fairly variable between patients. Also, there are probably 20 to 30 commercially available PRP systems on the market now. None of these produce PRP in exactly the same way, once again, making the argument that PRP injections cannot be completely standardized. For this reason, insurance companies often take a pass on something they don’t view as uniformly the same treatment for every patient.
Now, let’s turn attention to why it really may not matter whether insurance companies cover PRP or not and why you should not be deterred from seeking this treatment.
-First, let’s look at the financial piece. So many of our private insurances require that we first meet our deductible before insurance will pay a significant portion of our medical bill. These deductibles are rising. Until you meet your deductible, you are going to pay out-of-pocket for any office visit, diagnostic test, medical procedure, or medication. Therefore, let’s say you were choosing between a steroid injection versus a platelet-rich plasma injection. Technically, the steroid injection is “covered by your insurance,” but until you meet that deductible, you are going to pay for an office visit and the cost of that steroid injection. So, “covered by insurance” doesn’t mean it’s an expense-free treatment.
-Next, that steroid injection may not be the best treatment for your particular condition. Let’s say you have a partial rotator cuff tear. You either don’t want or don’t need surgery for it. The steroid injection may temporarily alleviate symptoms, but certainly will not heal the partially torn tendon, and in fact, some patients worsen within weeks to months after a steroid injection. Thus, assuming you then are still seeking care for your shoulder pain and torn tendon, you will require additional tests and treatments. This may mean an MRI, a long course of physical therapy, additional medication, or even surgery. Those options, especially when combined, can be very expensive. Although platelet-rich plasma injections are not covered by insurance, they could be the long-term solution to your problem, saving you hundreds to thousands of dollars on other necessary potential treatments. Therefore, why not choose the treatment that will be most successful, not just the one that your insurance states that it covers?
-Finally, gone are the days that you can depend on insurance companies decide what is best for you and your health. I tell patients all the time that I literally could give them 10 steroid injections over the course of the year and cause bodily harm to them and their particular joint or tissue. Insurance companies would reimburse me to do this, often without question. Nevertheless, that is just not the right thing to do. I took an oath as a physician to “first do no harm” which I have continued to practice to the best of my ability. In addition, not only do I want to not do harm, but I also truly desire to help my patient. Therefore, I will help you choose what I believe to be the best and most customized treatment option for your particular situation. This is not always in line with what insurance companies would prefer that I do. I have no desire to be a “rogue” physician, but I’ve dedicated my career to developing an expertise to help my patients. Part of our ability to help our patients lies in the fact that we get to know them personally and their particular situations, goals, desires, comorbidities, and even their financial situations. Therefore, we work as a team with our patients to decide what we believe is best for them. Although it’s very natural to want to pay as little as possible but still get the best outcome, you just can no longer rely on insurance companies to have the authority over these decisions for you.
I realize what is said above gives you a lot to consider. I have a passion for educating our patients on the best treatments for their particular situation, and I am dedicating to doing that for the remainder of my career.
As always, please let us know if we can be of assistance to you!
F. Clarke Holmes, M.D.
Impact Sports Medicine and Orthopedics